Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111
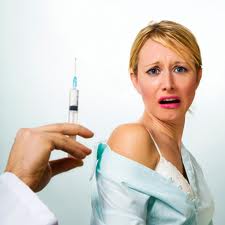
IN THE NEWS: Is This the Deadliest Vaccine on the Market? While the cervical cancer rate in the U.S. is 12 per 100,000, by Merck’s own admission, Gardasil may cause 2,300 serious adverse events per 100,000. Many of the more serious side effects of Gardasil vaccination are immune-based inflammatory neurodegenerative disorders, suggesting something is causing the immune system to overreact in a detrimental way, sometimes fatally. One of the leading theories is that the aluminum adjuvant in Gardasil is causing it to be excessively reactive. Data show Gardasil is several times more reactive than any other vaccine on the market. Trial data from Merck shows Gardasil may increase your risk of cervical cancer by 44.6 percent if you have been exposed to HPV strains 16 or 18 prior to vaccination. As of 2018, about 13,240 new cases of cervical cancer will be diagnosed, and about 4,170 will die from it. If you get regular Pap smears, your chance of dying from cervical cancer is 0.00002 percent. These seem like extraordinary risks just to prevent an infection that is cleared by more than 90 percent of people without a problem As noted in a film, the HPV vaccine’s underlying technology was originally developed by National Institutes of Health (NIH) researchers, then sold to Merck and fast-tracked to licensure, despite the fact the vaccine failed to fulfill two of the criteria for fast-tracking. It’s also important to realize that Gardasil was approved after being tested in fewer than 1,200 children under the age of 166 and that bioactive aluminum “controls” are being used in clinical HPV vaccine trials, thereby masking neurological symptoms.

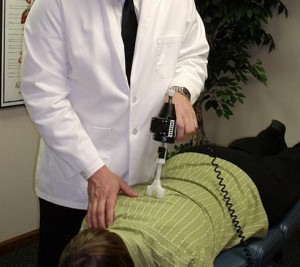
WELLNESS: Tendonitis: Its Causes, Symptoms and Treatments Tendons, which are flexible, tough and fibrous, connect your muscles to your bones. Muscles and tendons work together to exert a pulling force that helps you move properly. Tendonitis is an acute condition that occurs when injury to a tendon causes swelling and pain. It mainly affects your elbows, wrists, fingers, thighs, shoulders, knees and Achilles heels. There are two main tendonitis causes: sudden major injuries and repetitive movements over a time period while doing activities like: Gardening-Raking and shoveling-Carpentry-Cleaning or scrubbing-Painting-Throwing and pitching. Take note of these other factors that can increase a person's tendonitis risk: Age — Adults, especially those over 40 years old, are more injury-prone and have less-flexible and less-elastic tendons. Playing sports — Bowling, running, swimming, tennis, basketball, baseball or golf involve repetitive motions that can affect tendons. Health conditions — People with diabetes, rheumatoid arthritis, gout, psoriatic arthritis or thyroid disorders, those who experienced unusual reactions to medications, or people with hand or finger infections from cat or dog bites have a higher tendonitis risk. Body structure and posture — Tendonitis risk is higher with poor overall posture. Jobs or profession — Tendonitis is frequently seen in people whose jobs require them to stay in awkward positions, perform repeated actions, reach overhead, vibrate or forcefully exert their body. NOTE: Chiropractic helps.
CHIROPRACTIC: Although doctors of chiropractic treat more than just back pain, many patients initially visit a chiropractor looking for relief from this pervasive condition. In fact, about 31 million Americans experience low back pain at any given time. Interesting Facts about Back Pain Worldwide, back pain is the single leading cause of disability, preventing many people from engaging in work as well as other everyday activities. Back pain is one of the most common reasons for missed work. One-half of all working Americans admit to having back pain symptoms each year.3Back pain accounts for more than 264 million lost work days in one year—that’s two work days for every full-time worker in the country. Experts estimate that up to 80% of the population will experience back pain at some time in their lives.5Back pain can affect people of all ages, from adolescents to the elderly. Back pain is the third most common reason for visits to the doctor’s office, behind skin disorders and osteoarthritis/joint disorders. Most cases of back pain are mechanical or non-organic—meaning they are not caused by serious conditions, such as inflammatory arthritis, infection, fracture or cancer. Most people with low back pain recover, however, reoccurrence is common and for a small percentage of people, the condition will become chronic and disabling. Worldwide, years lived with a disability caused by low back pain have increased by 54% between 1990 and 2015. Low-back pain costs Americans at least $50 billion in health care costs each year—add in lost wages and decreased productivity and that figure easily rises to more than $100 billion.

FUNNY BONE:. Q: What do you get when you cross a dinosaur with a pig? A: Jurrassic Pork.@@Q: What animal should you never play cards with? A: A cheetah!@@I went down the street to a 24-hour grocery store. When I got there, the guy was locking the front door. I said, "Hey! The sign says you're open 24 hours." He Said, "Yes, but not in a row!"@@Boy: The principal is so dumb! Girl: Do you know who I am? Boy: No... Girl: I am the principal's daughter! Boy: Do you know who I am? Girl: No... Boy: Good! *Walks away*@@Molecule 1: I just lost an electron. Molecule 2: Are you sure? Molecule 1: I’m positive.@@ When Magnesium and Oxygen started dating I was like, "O MG!"
Visit our web sites: keefeclinic.com & facebook.com/keefeclinic

CLICK TO ORDER
Winter time humidity is a big issue. As the weather turns colder and the heaters start working 24/7 then the indoor air will start drying out.
Studies have shown that dry air has four main effects on the human body:

CLICK PIC
- Breathing dry air is a potential health hazard which can cause such respiratory ailments as asthma, bronchitis, sinusitis, and nosebleeds, or general dehydration since body fluids are depleted during respiration.
- Skin moisture evaporation can cause skin irritations and eye itching.
- Irritative effects, such as static electricity which causes mild shocks when metal is touched, are common when the air moisture is low.
- The "apparent temperature" of the air is lower than what the thermometer indicates, and the body "feels" colder.

CLICK PIC
As your body fights the dry air you start to use up your vitamin A stores. This enhances the dry skin and sinus problems as well as weakens your immune system. It is important that you have a humidity gauge in each bedroom and a cool mist humidifier to combat the dry air. I recommend the ultrasonic humidifiers as they put the most water in the air.

Some Of The Physical Effects Of Dry Air
Dry skin, Chapped lips, Clogged sinuses, Itchy skin, Dry throat coughs, Cracked nasal membranes, Increased risk of bacteria infection, Aggravated asthma & allergy symptoms
You may also notice these changes around your home:
- Woodwork and furniture shrinkage
- Hardwood floor separation
- Piano goes out of tune
- Wallpaper peels at the edges
- Drawers loosen
- Moldings gap
- Collectibles shrink, warp and crack
- Static Electricity increases

CLICK PIC
Drier air causes sinuses to dry and crack, making people more susceptible to winter colds and flu viruses. In fact, this change from higher outside relative humidity to lower indoor relative humidity in the winter is a significant contributing factor in the spread of colds and flus. By maintaining the proper level of humidity indoors, you reduce illness in the winter. Studies have shown that the body's immune system will function better when the relative humidity in a home is between 45%-65%.

CLICK PIC
Pneumococcus, staphylococcus, and streptococcus bacteria die up to 20 times faster at a relative humidity between 45% and 55%, than above 70% or below 20%. Dehydration can also cause negative health effects. Symptoms of dehydration include dry skin, chronic joint and muscle pain, raspy throat, sinus and nasal pain, sore eyes, a lack of mental concentration, and a decrease in the body's immune system.
| The most comfortable relative humidity for the human body |
45-65%RH |
| Ideal relative humidity for prophylactic and curative purposes |
40-50%RH |
| Computer and telecom apparatuses |
45-65%RH |
| Furniture and musical instruments |
40-60%RH |
| Libraries (books), art galleries and museums |
40-60%RH |
Quick Fix 1: Get Steamy

CLICK TO ORDER
Dry air can cause or irritate sinus problems, but inhaling moisture can help. Simply breathing the steam from a hot shower will ease congestion.

CLICK TO ORDER
You can also enhance the steam you breathe with sinus-clearing essential oils. Once or twice a day, add five drops of eucalyptus (Eucalyptus globulus), lavender (Lavandula angustifolia), or sandalwood (Santalum album) essential oils (or a combination) to a large bowl of steaming-hot water, suggests Sylvia Goldfarb, Ph.D., of Wyncote, Pa., author of Allergy Relief (Avery Penguin Putnam, 2000). Drape a towel over your head and the bowl, and breathe deeply for 10 minutes. You'll feel relief within that time.

CLICK TO ORDER
To treat acute sinusitis, substitute tea tree oil (Melaleuca alternifolia) and repeat the sinus steam three to four times daily. Tea tree oil's powerful antibacterial properties fight the bacteria that cause many infections," says Karen Barnes, N.D., a naturopath in Burlington, Ontario, and author of Naturopathic First Aid (Quarry Press, 2001). Your symptoms should clear up within a few days.
Quick Fix 2: Flush Your Sinuses
Rinsing your sinuses with saltwater helps them drain mucus. Studies show that this significantly reduced symptoms like pain and inflammation in more than 2/3 of sinusitis sufferers. Heatley says recommending nasal irrigation to her patients cut the number of sinus surgeries she performed in half.

CLICK TO ORDER
To rinse your sinuses, use a neti pot, a small teapot-like device sold at most natural food stores. Combine three parts non-iodized salt and one part baking soda, and add 1/2 teaspoon of this mixture to 1/2 cup of warm water in the pot. This solution matches your body's salinity, and baking soda makes it less irritating to your sinuses.
Lean over a sink and insert the spout of the pot into your left nostril. Tilt your head and the pot to the right and let the solution flow out your right nostril. Exhale forcefully through both nostrils and repeat on the other side. Repeat as needed.
Quick Fix 3: Eat Spicy Food

CLICK TO ORDER
The zing of certain spices opens clogged sinuses and promotes drainage. As condiments, use hot salsas or chutneys that contain chiles, or sprinkle cayenne pepper on your food, recommends Goldfarb or use wasabi.


CLICK PIC
Car accidents are most likely the number one cause for chronic disability and/or pain. The August 1999 issue of American Family Physicians, the article notes that 3.5 million people are injured in motor vehicle accidents in the U.S. each year. Even minor car accidents can cause changes in the spine that can lead to degenerating joint disease and future pain. Studies indicate that chiropractic care is the best treatment for the vast majority of injuries from a car accident. The main reason that chiropractic patients have less problems in the future and recover better from their present complaints is because of the focus in chiropractic care.
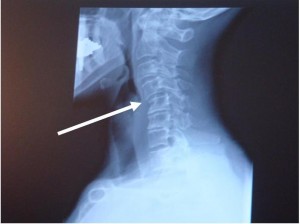
CLICK PIC
The injuries to the spine will cause slight misalignments in the joints of the neck and back. It's these misalignments that produce the majority of symptoms, not pulled muscles. Chiropractic care and analysis focuses on the detection and correction of spinal subluxations. Subluxation is the term for misalignments that develop in the spine. These misalignments can stay there for years unless they are corrected by chiropractic adjustments. The average patient after a car accident that visit an emergency room usually are only given pain pills and muscle relaxers. This of course allows the misalignments to remain. It's this focus on just the symptoms of the injury that leave a high percent of car accident victims with ongoing disability, pain and degenerating joint disease.
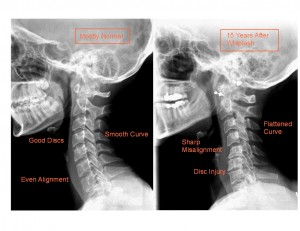
CLICK PIC
One study showed problems five or more years after the accident. Symptomatic recovery occurred in 57 per cent of the 146 patients, while degenerative changes developed after the injury in 39 per cent. Journal of Bone and Joint Surgery, 1974;56:1675-1682.
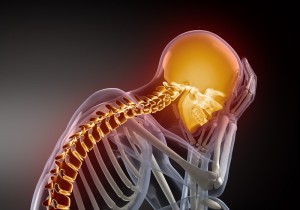
CLICK PIC
......several studies have investigated and linked the relationship of altered cervical curve configuration to the presence of chronic headache pain. CBP Structural Rehabilitaion of the Cervical Spine, Deed E. Harrision, DC, Donald D. Harrison, PhD, DC, MSE, Jason W. Haas, DC, 2002 Harrison CBP Seminars, Inc. pg. 56, "Cervical Lordosis and Headaches"

CLICK PIC
Cerebral symptoms after whiplash injury of the neck: a prospective clinical and neuropsychological study of whiplash injury. Ettlin TM, Kischka U, Reichmann S, Radii EW, Heim S, Wengen D, Benson DF. University Clinics, Basel, Switzerland.
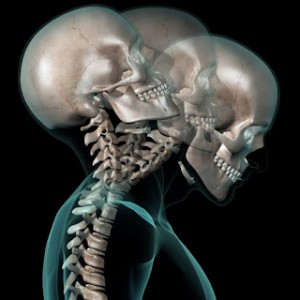
CLICK PIC
Twenty one unselected patients with an acute whiplash injury of the neck had neurological and neuropsychological assessment, cervical x rays, EEG, BAEP, MRI, and an otoneurological examination within two weeks of the injury. Subjectively, 13 patients reported concentration deficits, 18 reported sleep disturbances, 9 had symptoms of depression, and 7 female patients told of menstrual irregularities. Scientific Automobile Accident Reconstruction treatise by Barzeley; Published by Mathew Bender 1984; Chapter 46:
" The simple fact remains: neck injuries do occur as a result of rear-end automobile accidents. 46-2
" Whiplash injuries may be present as a result of automobile accidents, even though no physical, radiological or other objective evidence of injury can be found. 46-3
" Usually the onset of symptoms occurs from 12 to 24 hours afterward. Sometimes there may be as much as weeks or even months delay between the automobile accident and the experience of symptoms. 46-5
" Most people just don't expect injuries to occur when the impact velocity has been low and damage to the vehicles has not been great. It is common sense to expect that the severity of the injuries should be in proportion to the severity of the collision. However, whiplash injuries most frequently result from relatively minor automobile accidents without major damage done to the vehicles. 46-6
" Rear-end collisions produce a sudden forceful hyperextension of the neck which is immediately followed by recoil into neck flexion. 46-8
" Probably most of the injuries result from the sudden traumatic snapping of the neck when the acceleration of the head suddenly shifts directions. 46-10
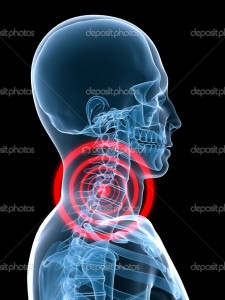
CLICK PIC
In most cases you're better off in the long-term to break a bone than to damage a joint. When you damage a joint, you primarily damage the connective tissue in the joint which can leave that joint unstable for the rest of your life. When you break a bone, the bone heals stronger than it was before. Connective tissue has a history of poor healing. By bringing that joint back to its proper alignment, you allow the maximum healing to the soft tissue or connective tissue in that joint. And by maintaining that alignment over the long-term, you assure maximum results. Out of 50 or so outcome studies which have been published in the past 40 years. They nearly unanimously presented 30 to 50 percent of whiplash victims are left with some form of residual pain or dysfunction.
Our treatment goals are not only to make you feel better now, but to try to assure that 10 years from now your injuries will not be bothering you.
CLICK PIC
CLICK PIC
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111

IN THE NEWS: CDC warns parents not to give children antibiotics to treat the common cold, flu "Antibiotics are not effective against viral infections like the common cold, flu, most sore throats, bronchitis, and many sinus and ear infections," read a recent CDC advisory on Facebook. "Taking antibiotics can also have harmful side effects for you or your child." While parents might be tempted to seek out antibiotics during this year's supposedly more severe than usual flu season, taking the bacteria-killing medication will not cure the infection, stop others from catching it, nor make flu victims feel better. In fact, needlessly taking antibiotics will kill healthy bacteria and may lead to harmful side effects that could send a child to the hospital. According to the CDC, antibiotics are the most common cause of emergency hospital visits for children experiencing negative reactions to drugs. In addition, needlessly using antibiotics can make the body more resistant to the medication, making it harder to treat an infection. In total, the CDC estimates that 30 percent of all antibiotics prescribed to patients seeking medical treatment without hospital admission are unnecessary.

CHIROPRACTIC: American Chiropractic Association (ACA) has announced a national health care observance--October is National Chiropractic Month DO YOU KNOW SOMEONE WITH A HEALTH PROBLEM OR IN PAIN? INVITE YOUR FAMILY OR FRIENDS TO THE PARTY Who do you know who is hurting? Who do you know that you have been trying to get started at Keefe Clinic? Now is the time to get your spouse or child started on the road to good health. Complimentary DIAGNOSTIC WORK UP DURING OCTOBER Complimentary initial exam and one X-ray. Tell someone today

WELLNESS: Empathy: Caring for Others Is Good for You Empathy, the ability to put yourself in someone else’s shoes, so to speak, and understand their feelings and point of view, is a character trait that may benefit society and individuals in multiple ways. Empathy training has been found to reduce stress levels among medical students facing intense emotional encounters with patients, for example. While many parents try to instill empathetic qualities in their children, there’s growing research that empathy has deep neurological roots in humans. Empathy has complex neurological underpinnings that control the way our brains help us to care about other people. Humans have “mirror neurons” that react to others’ emotions and reproduce them; a deficit in mirror neuron receptors has been suggested as an explanation for narcissism and neurotic behaviors. Researchers found that empathy was positively associated with treatment adherence, patient satisfaction and reduced dental anxiety, sentiments that seem to be echoed among medical practitioners. Among adolescents, empathy may even go hand in hand with future success, according to licensed professional counselor Ugo Uche: “Teenagers who are empathetic tend to be more purpose driven and they intentionally succeed in their academics not because they are looking to make good grades, but in most subjects their goal is to understand the subject material and to utilize the knowledge as one of their ever-increasing tools …Teenagers who are more empathetic do a much better job in embracing failure, because there is little ego involved in their tasks, and setbacks while disappointing are rarely seen as failures, but rather as a learning experience about an approach that does not work for the task at hand.” Practicing empathy may help you relieve stress, strengthen your relationships and have a more satisfying work life.
FUNNY BONE: The last time we changed from daylight saving time, a preacher friend posted, “For those who habitually show up 15 minutes late to church, allow me to remind you that tonight is the night you set your clock back 45 minutes.”@@ Q: What starts with E, ends with E, and has only 1 letter in it? A: Envelope. @@ After an elderly couple starts getting forgetful, they visit their doctor. Their doctor tells them that many people find it useful to write themselves little notes. When they get home, the wife says, "Dear, will you please go to the kitchen and get me a dish of ice cream? And maybe write that down so you won't forget? “Nonsense," says the husband. "I can remember a dish of ice cream. “Well, I'd also like some strawberries and whipped cream on it," the wife replies. "My memory's not all that bad," says the husband. "No problem -- a dish of ice cream with strawberries and whipped cream. I don't need to write it down." He goes into the kitchen, and his wife hears pots and pans banging. The husband finally emerges from the kitchen and presents his wife with a plate of bacon and eggs. She looks at the plate and asks, "Hey, where's the toast I asked for?"
Visit our web sites: keefeclinic.com & facebook.com/keefeclinic
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111
IN THE NEWS: Which Foods Are Best for Your Heart Health? Many vegetables contain naturally occurring nitrates, which your body transforms into nitric oxide (NO), a soluble gas continually produced from the amino acid L-arginine inside your cells. nitric oxide supports healthy endothelial function and protects your mitochondria. Acting as a potent vasodilator, NO also relaxes and widens your blood vessels, improving blood flow and reducing blood pressure. As noted in research3 presented by Dr. Michael Greger above, a diet high in nitrate is a natural strategy recommended for the treatment of prehypertension and hypertension (high blood pressure), "and to protect individuals at risk of adverse vascular events," i.e., heart attacks. Indeed, raw beets — which are high in nitrates — have been shown to lower blood pressure by an average of four to five points within a matter of hours. Some studies have shown a glass of beet juice can lower systolic blood pressure by more than eight points — far more than most blood pressure medications. In conventional medicine, nitrates are used to treat angina and congestive heart failure, and research shows a glass of beetroot juice has the same effect as prescription nitrates. Red beets are well-known for their high nitrate content, but leafy greens contain even more nitrates per serving; arugula contains the highest amounts, followed by rhubarb.

WELLNESS: Sugar During Pregnancy Linked to Allergies Allergies are a sign your body’s immune system is working overtime; consuming sugar during pregnancy may increase your child’s risk of developing allergies and asthma. Sugar has a profound effect on the health of your growing baby and may increase your own risk of obesity, metabolic syndrome, hypertension and brain-related disorders as well. Researchers at Queen Mary University of London evaluated survey data from nearly 9,000 mother-child pairs in the ongoing Avon Longitudinal Study of Parents and Children, tracking the health of families with children born between April 1, 1991, and December 31, 1992.4 Lead author Annabelle Bedard, Ph.D., commented on what triggered the researchers to evaluate the association between sugar and allergies: "The dramatic 'epidemic' of asthma and allergies in the West in the last 50 years is still largely unexplained — one potential culprit is a change in diet. Intake of free sugar and high fructose corn syrup has increased substantially over this period. We know that the prenatal period may be crucial for determining risk of asthma and allergies in childhood and recent trials have confirmed that maternal diet in pregnancy is important." Optimizing your vitamin D level during pregnancy may reduce your child’s risk for developing asthma and support your child’s immune system.
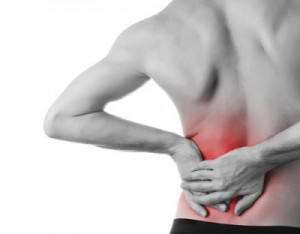
CHIROPRACTIC: Low back problems that are disc related Low back pain is the number one health problem in the United States, but the good news is chiropractic is the number one effective treatment based on government studies. When vertebrae, in the back, start to lose their alignment, the connective tissue and fluid pad (discs) between the vertebras come under stress. Through repetitive trauma from normal daily activities, this stress can lead to bulging and sometimes tearing of fibers within the disk. As this damage increases the gelatinous material called the nucleus pulposus can migrate to the edge of the disc and sometimes herniated through the disc. The good news is most disc problems can be adequately resolved through chiropractic adjustments, exercise, and nutritional therapy. That's right, discs need nutrition just like every other structure in your body. With a combination of connective tissue support, enzymes to treat inflammation and swelling and chiropractic adjustments most disk problems can be resolved without surgery. There is a classic disc shift seen in patients with lumbar disc disorders. When the patient tries to stand up straight, their hips are usually shifted to one side. If you or someone you know suffers from severe low back pain, they need chiropractic care to resolve the disk problem.

FUNNY BONES: How does a penguin build it's house? Igloos it together. @@Bob: "Holy schmoozes, I just fell off a 30 ft ladder." Jim: "No way man, are you okay?" Bob: "Yeah, luckily I was just on the first step."@@Two years ago I asked the girl of my dreams on a date, today I asked her to marry me. She said no, on both occasions.@@police say that the man who fell into a combine harvester while trying to steal it…Has been bailed. @@I told a girl she looked better without her glasses on. She said I also look better without her glasses on.@@“Dad, are we pyromaniacs?” “Yes, we arson.” @@To the guy who stole my antidepressants…I hope you’re happy.@@I asked the doctor if I could administer my own anaesthetic. He said, “Go ahead. Knock yourself out.” @@I’ve been trying to organize a hide and seek tournament…But it’s not easy. Good players are hard to find.@@ A guy walks into library and asks for a book on sea turtles. The librarian asks, “Hard back?” The guy replies, “Yeah, little heads too.”
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111
IN THE NEWS: Researchers Uncover Link Between Immune Function And Osteoarthritic Pain And Progression The immune system plays a pivotal role in the amount of pain and disease progression experienced by patients with osteoarthritis (OA), McMaster University researchers have found. This discovery could lead to new strategies for improving joint pain management and immune function in older adults with arthritis. The study, published in the medical journal Osteoarthritis and Cartilage, found that monocytes, the white blood cells necessary to regulate immune responses, were more activated and pro-inflammatory in women with osteoarthritis, and that elevated inflammation and body mass index were associated with this increased activation. When compared with a control group, this combination created a perfect storm – one that was found to increase the pain and progression of knee osteoarthritis. The study involved 22 women with OA, and 22 women of the same age without OA.NOTE: Monocytes are usually elevated in response to bacteria and parasites. Recently study show that rheumatoid arthritis can be triggered in some cases by a bacteria in milk. Nutritional formulas that enhance immune function allow for the body to eliminate these microorganisms and begin the healing process. Detoxification, anti-inflammatory diet are just some of the things that can be helpful in health recovery.
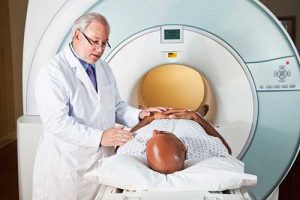
WELLNESS: Chuck Norris Focuses Attention on Heavy Metal Risks After Enhanced MRI Magnetic resonance imaging (MRI) is a study allowing your physician to see detailed images of your organs and tissues using a large magnet and radio waves. Gadolinium-based contrast agents (GBCAs) may be prescribed to enhance the image but the heavy metal gadolinium is known to deposit in your brain, bone and organs. The FDA acknowledges the metal may be found in your tissues for years but claims there is no known effect, despite the rising number of people suffering from kidney damage, cognitive dysfunction and muscle wasting. Strategies you may consider if an enhanced MRI is absolutely necessary include optimizing your gut and nutrition, eating fermented foods and using a sauna to aid detoxification. After undergoing three MRIs with GBCAs to evaluate her rheumatoid arthritis, Gena O'Kelley, the wife of American film icon Chuck Norris, began experiencing severe physical symptoms that began with a burning sensation in her skin. She described it as if there was acid burning her skin, slowly covering her body. She reports that she visited the emergency room five or six nights in a row, while doctors ran multiple tests for ALS, MS, cancer and Parkinson's disease. However, it was O'Kelley who made the connection between her burning skin, contracted arm and cognitive issues and the multiple MRIs she had undergone. She told Full Measure: "When we got to the hospital in Houston this last time, and I'm so bad and I said, listen, I am sober enough in my thinking right now, because I had such brain issues going on, I said I'm only going to be able to tell you this one time and I need you to listen to me very closely. I have been poisoned with gadolinium or by gadolinium and we don't have much time to figure out how to get this out of my body or I am going to die." After five months of treatment in China and then in a clinic in Nevada, O'Kelley was able to return home to her seven children for continued treatment by a physician in Houston. Norris shared their tax return records documenting $2 million over three years in uninsured medical expenses to help O'Kelley return to health. Now Norris is suing 11 medical companies for the part they played in not warning the couple and others of the dangers of using a GBCA for MRI contrast.
CHIROPRACTIC: IMMUNE FUNCTION studies of chiropractic patients have shown interesting differences with those patients that have ongoing chiropractic care and just the average person off the street. One of those differences we have discussed in a past newsletter about DNA repair. Those who have gotten regular chiropractic adjustments have a higher level of a chemical that’s involved in repair of DNA. Our DNA is traumatized hundreds if not thousands of times during the day and repair of DNA is essential in longevity and health in general. Many years ago an immunologist studying chiropractic patients who receive regular care were found to have an immune system operating 400% better than the average person on the street. The nervous system regulates and controls every system in your body and misalignments depress function including immune function. When you receive an adjustment you improve nervous system control and coordination over your immune system. Keeping a healthy immune system requires a clean diet, plenty of fluids, exercise, proper rest and a healthy nervous system. Increase your immune function through regular chiropractic care.
 |
FUNNY BONE: When my three-year-old was told to pee in a cup at the doctor’s office, he unexpectedly got nervous. With a shaking voice, he asked, “Do I have to drink it?”@@ Probably the worst thing you can hear when you’re wearing a bikini is “Good for you!”@@ A couple years ago my therapist told me I had problems letting go of the past.@@ "Doctor, there's a patient on line 1 that says he's invisible" "Well, tell him I can't see him right now."@@ Dr.'s are saying not to worry about the bird flu because it's tweetable.@@ When an employment application asks who is to be notified in case of emergency, I always write, "A very good doctor".@@ I grew a beard thinking it would say "Distinguished Gentleman." Instead, turns out it says, "Senior Discount, Please!"
| Visit our web sites: keefeclinic.com & facebook.com/keefeclinic |
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111

IN THE NEWS: Wide Awake in the Electronic Age: Our Kids' Sleep Habits Are Suffering Smartphones, tablets and everything in between – chances are high that if your child's over the age of 6 (and in some cases, even younger these days), they're spending a considerable (read: unhealthy) amount of time engaged with portable electronic devices. At the same time, we're finding that kids are suffering from sleep deprivation in terms of time spent asleep and quality of sleep enjoyed. Is there a connection? Yes, say researchers who reviewed various studies on the topic – and the news is even worse than you might imagine. After reviewing 20 studies, researchers found that kids who used portable electronic devices near bedtime had more difficulty falling or staying asleep, and experienced poor daytime function because of sleepiness. Device use also contributed to lack of sleep compared to non-use: less than 10 hours per night for children and less than nine hours for teens. But here's the kicker: Even kids who didn't use the devices, but had access to them, still experienced shorter sleep times. Children with bedtime access to devices close to bedtime three or more times a week also experienced less sleep and lower quality of sleep compared to children with less or no device access. Researchers speculate that access, even without use, can exert an influence on sleep because children are thinking about different aspects of the device, such as text messaging (e.g., "Has someone responded to that message I sent earlier?").

WELLNESS: Exercise: The Key to Better Grades? For better or worse, we live in an increasingly competitive world, which means when it comes to education, grades matter – big time. While they don't necessarily reflect the learning process, effort expended or lessons learned, grades remain an important indicator of knowledge, critical thinking and other variables that translate well into adulthood. And of course, when applying for college, few application reviewers consider the straight D student, even if that student gave 100 percent in the classroom every day. With all the tutoring clubs, online support groups and other tools at students' / parents' disposal these days, it's encouraging to know a simple grade-booster exists that doesn't require money or even a great deal of extra time: exercise. Research suggests children who exercise more perform better in several academic subjects and are more attentive compared to their less-active peers. The most recent study to examine this association reviewed 26 studies involving more than 10,000 children ages 4-13. Results, published in the peer-reviewed research journal Pediatrics, showed that increased physical activity, particularly physical education, improved various aspects of academic achievement , "especially mathematics-related skills, reading, and composite scores." Students who exercised more also appeared to stay more focused on their schoolwork than students who exercised less. In the studies analyzed, researchers increased physical activity levels through expanded recess, afters-school sports or active breaks between lessons throughout the school day – which also may suggest academic performance is related to whether kids get breaks from their long days sitting in the classroom. Definitely food for thought for the education system. From a parent standpoint, teaching your kids to exercise and encouraging them to take active breaks at home, particularly while doing schoolwork or studying for quizzes / tests, could help their academic performance – and will certainly help avoid the health perils of a sedentary lifestyle. Talk to your doctor for more information.
CHIROPRACTIC: Kids and Chiropractic Care “Chiropractic care for my child? Why? His back doesn’t bother him.” How often chiropractors have encountered parents who appreciate the importance of regular checkups for their child’s teeth, hearing, eyes and ears but draw a blank when it comes to a spinal checkup. In fact, a spinal check up could be one of the most important checkups your child will ever have. Your child’s spine is his/her lifeline because running through it is the spinal cord, containing billions of nerve fibers that send messages and energy from the brain to every part of their body. If there is blockage of any of the nerves along the spinal cord, any nerve damage at all, then a state of ” dis-ease” will develop. Dis-ease means dis-harmony in the body that will cause generalized weakening of your child’s body, lowered resistance to disease, and consequent body malfunction and sickness. Blockage of nerves in the spinal column are usually caused by tiny fixations and misalignments of the spinal vertebrae that are called vertebral subluxations. Only chiropractors are trained to detect and correct subluxations, much like only a dentist finds cavities. Subluxations can be cause by the birth process, the very physical childhood activities of running and jumping, falls and accidents. Because your children (and you) may have spinal subluxations and not know it, all children need periodic spinal check ups. A recent study of 332 children showed that chronic ear infection sufferers under chiropractic care had no more infections in 80% of the cases (JCCP, Vol.2, No.2 1997). The Chiropractic Approach By releasing stress on the nervous system with very gentle and safe chiropractic adjustments, the body will work more effectively and be able to express better health. Why not include chiropractic spinal checkups for you and your children? It may be the best move for your family’s health you’ll ever make.

FUNNY BONE: With tears in his eyes, the little boy told his kindergarten teacher that only one pair of boots was left in the classroom and they weren’t his. The teacher searched and searched, but she couldn’t find any other boots. “Are you sure these boots aren’t yours?” – she asked. “I’m sure,” the little boy sobbed. “Mine had snow on them.”@@ My little sister is so smart! She’s only in nursery school and she can spell her name backwards and forwards. Really? What’s her name? Anna.@@During Show and Tell, Miss Johnson showed pictures of different birds. “George,” she said, “what kind of bird do you like best?” George thought for a while. “Fried chicken,” he replied.@@“It’s clear,” said the teacher, “that you haven’t studied your geography. What’s your excuse?” “Well–my dad says the world is changing every day. So I decided to wait a little while until it settles down.”@@ “No one likes me at school,” said the son to his mother. “The kids don’t and the teachers don’t. I want to stay home.” “You have to go, son,” insisted his mother. “You’re not sick, and you have a lot to learn. Besides, you’re 45 years old. You’are the principal and you have to go to school!”
Visit our web sites: keefeclinic.com & facebook.com/keefeclinic
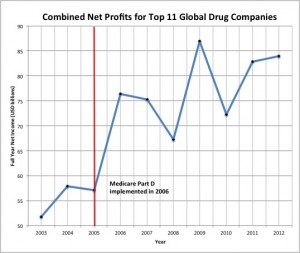
I don't keep up with drug sales let alone the actions and side effects of all the latest drugs. But I would think antacids must be making pharmaceutical companies literally billions of dollars each year. (The January 8, 2001 issue of Business Week mentions that Priolsec is the top selling prescription drug in the world. It earns Astra Zeneca (the drug’s maker) 6 billion dollars per year.)
CLICK FOR INFO
CLICK FOR MORE
One of the reasons that antacids sell so well is that they stop the pain in 60-70% of the cases. (A recent online survey of over 4200 patients taking Priolosec.) If you're troubled with chronic acid reflux and you can take a pill and all the pain just disappears, it seems like you're doing the right thing, doesn't it? Before you answer that let me explain the digestive process and then ask you that question again.
Digestion is literally a miracle. All the different types of foods and yet your body knows the exact enzymes and the correct amount to properly breakdown each food to its simplest component. Complex carbohydrates are broken down into simple sugars, proteins are broken down into their individual amino acids and fats and oils are reduced to their individual fatty acids. And then the process of properly absorbing these nutrients along with the vitamins, minerals and enzymes plus other things that were still learning about. If you eat different foods you get different kinds and amounts of enzymes to digest them.
CLICK FOR MORE

CLICK HERE
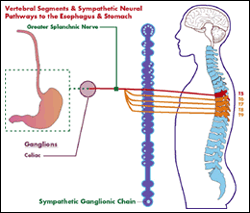
As you chew your food you help break it down for your stomach as well as blend it with saliva which helps start the whole process. As the food enters the stomach it starts to churn and release digestive enzymes. Hydrocloric acid (HCl) is one of the most important enzymes that the stomach releases. The amount of HCl that leaves the stomach with the food entering the small intestines stimulate fluids from the liver and gallbladder as well as enzymes from the pancreas to complete the digestive process. It is essential that the right amount of HCl enters the small intestines to begin a wavelike motion called peristalsis that help move the food throughout the intestines. If the level of HCl is less than ideal then every other step in the digestive process is compromised.

CLICK HERE
It's like when you have a row of dominos stacked together and push the first one over a chain reaction happens. Without HCl the rest of the digestive process is severely compromised. If you don't produce the right amount of enzymes then you cannot breakdown your foods properly. If you don’t break your foods down properly you can not absorbe nutrients that your body requires. Studies of individuals who have used antacids over a long peiord of time find evidence of malnutrition. Doesn't that make sense? What do antacids do? They severely reduced if not completely block the release of HCl. Remember the chain of dominos.

CLICK HERE
When you consistently reduced the amount of HCl that is released from your stomach that causes a series of changes in the lining of your stomach. A healthy stomach has a mucous lining that protects the stomach from its own acids. When the body senses that this coating has been reduced it automatically reduces the amount of HCl it secretes. As this happens the stomach will churn more to help break down the foods. After a series of processes, this increase of abnormal stomach contractions can force what little bit of HCl you produce up into the esophagus.

CLICK HERE
This can cause a burning or painful sensation from your stomach up into the back of your throat. This is called acid reflux. This condition is rarely due to the overproduction of HCl. If this problem is not corrected over a lifetime the chronic inflammation to the cells can lead to cancer. But be forewarned, the chronic suppression of HCl with antacids will lead to incompletely digested food irritating your intestines and increasing your chance for colon cancer. Usually the mechanism I described above is leading to the inappropriate release of HCl into the esophagus. It is true eliminating the amount of HCl you produce will relieve symptoms. It's also true that these drugs will relieve you of the normal digestive process.

CLICK HERE
Now the main question is this- is the choice between symptom relieve with drugs or suffering pain with each meal? No! By properly correcting the dysfunction within the digestive system you can, not only restore proper function without drugs, you can also overcome your acid reflux.

CLICK HERE
There are several principles to good digestion. Completely chewing your food, not combining proteins with sweet fruits, don't eat too quickly, eat foods that are consistent with your body and blood type, too much dairy with a meal could interfere with the digestive process and watch the junk food. Fiber helps move the food through your digestive system.

CLICK HERE
A lot of time patients with digestive problems also notice that they have discomfort between the shoulder blades. Neurologically this is very significant. The nerves between the fourth thoracic and eight thoracic are some of the most important controlling nerves to your digestive system. If you carry nerve pressure in your upper back then your digestive system is most likely compromised. Now remember, you can have nerve pressure without back symptoms, though alot of patients with acid reflux know what I'm talking about when I talk about discomfort between their shoulder blades.

CLICK TO ORDER
B-vitamins are very important when it comes to digestion and because you can't store B-vitamins. A good percentage of patients with digestive problems also have deficiencies in some of their B-vitamins. We also use targeted nutritional formulas to help restore the normal lining of the stomach along with diet and Chiropractic adjustments.

CLICK HERE
The care I just outlined for acid reflux is also extremely beneficial from most other digestive problems. Chiropractic care is the most effective treatment on the planet for digestive disorders. Most other approaches, even with gastroenterologists, focus primarily on symptom relieve and not correction.

CLICK HERE
Now let me ask you that question again and tell me if you might have a different answer. If you're troubled with chronic acid reflux and you can take a pill and all the pain just disappears, it seems like you're doing the right thing, doesn't it? Are you?
Low back pain is the number 1 health problem in the United States and most Western countries. Both drugs and surgery have been shown to be inferior approaches in the treatment of low back pain.
91 people die every day because of opiate addiction started by a prescription given to them by their medical doctor for pain, low back pain being the most common. Medical doctors have minimal training in structural problems that’s why they throw drugs and surgery at the problem. In the 1990s the US government released a report to every doctor’s office and healthcare facility in the US concerning low back pain and recommending spinal adjusting as the number 1 active and effective treatment. Yet you will read below that supposedly most doctors are unaware of this. Drug therapy kills 2000 people a week based on Senate reports and that has been happening for as long as we have records and will only increase if change isn’t forced upon the medical profession. Here’s a summary of the report released by the government around 20 years ago.

The Agency for Health Care Policy and Research, a branch of Health and Human Services, reviewed all treatments for acute low back pain and developed the following conclusions:
Physical therapy is not cost effective.
Acupuncture is not effective.
Over the counter anti-inflammatory medication worked as well as prescription ones (Cox-2 inhibitors were not included in the study).
Sclerotherapy and Prolotherapy are not effective.
The use of cortisone injections should be used only in cases of sciatic pain which radiates down the leg and doesn’t respond to conservative therapy.
Surgery is over used and should be offered in less then 1% of cases.
Rest should be given initially for 24-48 hours.
Early movement that is tolerable should be initiated after 48 hours.
Cushioning in shoes can be helpful.
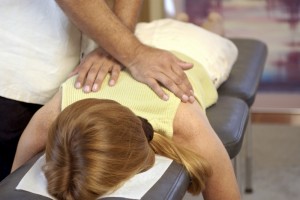
Spinal adjustments are the only active form of therapy given by a professional which is helpful.

Since most doctors and patients are not aware of this report, patients all around the country are needlessly suffering and being mistreated. There are many treatments available for severe back problems that have better short and long term benefits over spinal surgery, epidural injections and long term pain medications. Our office is aware of the latest advances and are free to discuss these alternatives with you. 918-663-1111
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111

IN THE NEWS: USING YOUR IPHONE, ANDROID AND KINDLE TO MONITOR YOUR HEALTH. QardioArm is a portable blood-pressure unit that allows you to check your blood pressure anytime. It helps keep track of your blood pressure by maintaining a history by location of each blood-pressure. QardioCore is the world’s first ECG monitor designed to provide continuous medical grade data while fitting your lifestyle. QardioCore is particularly suited for people with increased health risk caused by family predisposition, history of heart attacks or strokes, high blood pressure, high cholesterol, diabetes and excess weight. QardioBase Smart Scale is one of the best looking bathroom scales for your home, and one of the smartest. In addition to weight, Qardio App also tracks your BMI and full body composition changes over time so you can get to know your body better. QardioBase smart scale automatically and wirelessly syncs your measurements to your Qardio App. Simply step on the scale and QardioBase does the rest. Google Qardio.
WELLNESS: SIMPLE TOOLS TO MAINTAIN HEALTH IN A TOXIC WORLD. Maintaining health can be challenging in the world we live in. There are so many temptations to eat wrong, to maintain an inactive lifestyle as well as other poor health habits. The 1st thing we should look at is maintaining healthy function. Chiropractic adjustments help enhances function to every organ, part and system of body by reestablishing communication channels that have been blocked by misalignments. The next important principle is properly feeding the body the nutrients that it needs. There are different metabolism types that need to be addressed properly and that’s the principle of the “body type diet” system. Knowing your body type can go a long ways of maintaining proper nutritional and chemical balance. The next important thing is reducing inflammation in the body which again can be accomplished by targeting certain foods that put out the fire. There are certain powerful antioxidants in foods like pomegranate, blueberries etc. The next issue with inflammation is maintaining certain levels of EPA-DHA (fish oils) in your body to control inflammation. If your system is inflamed then most likely your urine pH is acidic. Drinking alkaline water will not only help with an acid pH but also enhances the next important step of detoxification. Our system can be overloaded with environmental toxins and toxins from internal metabolism that are not properly eliminated. Along with these types of toxins electromagnetic overload can also be an issue with your health. We offer multiple detox programs to help improve your body’s ecology. Simply drinking the right amount of water for your body weight goes a long ways of helping your body flush out toxins. Dehydration can be a source of many different health problems. Following these simple steps can eliminate many of the common diseases that our society is plagued with. You cannot drug yourself into better health because health is a “natural” process that is better served with natural healthcare. You are the one responsible for your own health but we can give you the direction to help you reach that goal.
CHIROPRACTIC: WHAT ARE CERVICOGENIC HEADACHES? Headaches are a very common problem that can have multiple causes ranging from stress to trauma. To make matters worse, there are MANY different types of headaches. One such type is the “cervicogenic headache” (others include migraines, cluster headaches, etc.). The main distinction between the symptoms associated with cervicogenic headaches and those associated with migraine headaches are a lack of nausea, vomiting, aura (a pre-headache warning that a headache is about to strike), light and noise sensitivity, increased tearing with red eyes, one-sided head, neck, shoulder, and/or arm pain, and dizziness. The items listed above are primarily found in migraine headache sufferers. The following is a list of clinical characteristics common in those struggling with cervicogenic headaches: Unilateral (one-sided) head or face pain (rarely is it on both sides). Pain is localized or stays in one spot, usually the back of the head, frontal, temporal (side) or orbital (eye) regions. Moderate to severe pain intensity. Intermittent attacks of pain that last hours to days. Pain is usually deep, non-throbbing, unless migraines occur at the same time. Head pain is triggered by neck movement, sustained awkward head postures, applying deep pressure to the base of the skull or upper neck region, and/or taking a deep breath, cough or sneeze can trigger head pain. Limited neck motion with stiffness. Infrequently, the cervicogenic headache sufferer can present with migraines at the same time and have both presentations making it more challenging to diagnose. The cause of cervicogenic headaches can be obvious such as trauma (sports injury, whiplash, slip and fall), or not so obvious, like poor posture. A forward head posture can increase the relative weight applied to the back of the neck and upper back as much as 2x-4x normal. Last month, we discussed the intimate relationship between the upper two cervical vertebra (C1 & C2) and an anatomical connection to the covering of the spinal cord (the dura) as giving rise to cervicogenic headaches. In summary, the upper three nerves innervate the head and any pressure on those upper nerves can result in a cervicogenic headache. Doctors of chiropractic are trained to examine, identify, and treat these types of potentially debilitating headaches.

FUNNY BONE: Two cows are standing next to each other in a field. Daisy says to Dolly, "I was artificially inseminated this morning." "I don't believe you," says Dolly. "It's true, no bull!" exclaims Daisy.@@ Went to the corner shop - bought 4 corners.
Military Pranks Are Scarier Than Bombs The military has a long, proud tradition of pranking recruits. Here are some favorites from rallypoint.com:
- Instructed a private in the mess hall to look for left-handed spatulas
- Sent a recruit to medical-supplies office in search of fallopian tubes
- Had a new guy conduct a “boom test” on a howitzer by yelling “Boom!” down the tube in order to “calibrate” it
- Ordered a private to bring back a five-gallon can of dehydrated water (in fact, the sergeant just wanted an empty water can)
Visit our web site: keefeclinic.com-ebook/keefeclinic.com
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111

DIET: How to Boost Brain Performance and Prevent Dementia Using No- or Low-Cost Strategies A diet that increases inflammation, such as one that includes high amounts of wheat, refined carbs and sugar is one of the root causes and greatest risk factors for Alzheimer’s disease; diet is also a foundational prevention and treatment strategy. To prevent Alzheimer’s, you need to focus on a diet that powers your brain and body with healthy fats, not net carbs. To shift your body into fat-burning mode, you need to dramatically reduce your net carbs, as your body will typically use whatever glucose is available first. However, that doesn’t mean you can never have large amounts of carbs ever again. In fact, remaining in nutritional ketosis for years on end may be ill advised. Alzheimer’s prevention and treatment is best approached from a holistic perspective. Besides a ketogenic diet, lifestyle factors that come into play include exercise, sleep, stress reduction, sun exposure and social interaction. Sleep can play a significant role in your brain health, as your brain can only detoxify and clean itself out during deep sleep.

IN THE NEWS: EPA Sued for Policy Many people are not aware that, in the U.S., dental offices are the single largest source of mercury at sewage treatment plants. When dentists discharge mercury from amalgam fillings (also known, misleadingly, as “silver” fillings) down the drains in their offices, it accumulates in the environment, including in seafood intended for human consumption. As a neurotoxin, mercury in the environment is dangerous for everyone, but poses a particularly grave risk for pregnant women, babies and children, in whom it can seriously disrupt brain function and harm the nervous system. In December 2016, the U.S. Environmental Protection Agency (EPA) finalized a rule that would restrict dentists' mercury discharges by requiring them to install amalgam separators. With the changes in administration, that rule has been rolled back, and the EPA is facing a lawsuit because of it. The Natural Resources Defense Council (NRDC) states the EPA rescinded the rule illegally, as it cannot be done without public notice or a comment period.

CONDITION OF THE WEEK: NUMBNESS IN THE ARM AND HAND if you or someone you know suffers from numbness in the arm or hand then you’re most likely dealing with the neck problem. Sometimes you might not have any symptoms in your neck yet the tiny bones in your neck could be pressing on the nerves that go down to your fingertips. Besides nerve pressure an unresolved whiplash can cause compression on the discs in the neck and as they break down put pressure on the nerves to the fingers. Realignment of the neck can resolve this condition along with shoulder problems, tennis elbow, carpal tunnel syndrome as well as numbness or swelling in the hand. It’s important to understand you can have nerve pressure without pain. If you or someone you know suffers from this condition have them call 918-663-1111.

FUNNY BONE: Andy has 150 candy bars. He eats 125. What does Andy have now?
Andy has diabetes now.@@ Whenever I’m sad I just read my blood donor ID. It always says “B positive”.@@ Oh, they were laughing when I told them I’m becoming a stand-up comedian. Well, ha! They’re not laughing now!”
Visit our web sites: keefeclinic.com & facebook.com/keefeclinic
In this terminology, “acute” stands for pain lasting fewer than four weeks, “subacute” for pain lasting from four to 12 weeks, and “chronic” meaning pain lasting more than 12 weeks.
The researchers conclude their findings with three recommendations, based on their assessment of evidence-based outcomes for the patient population with respect to standard noninvasive approaches to treatment. Namely, they examined how patients responded to pharmacologic treatment and nonpharmacologic treatment; in other words, standard allopathic medicine and complementary and alternative medicine (CAM).
The ACP recognizes that low-back pain is one of the most common health complaints in the U.S., and cite statistics with which every doctor of chiropractic (DC) is intimately familiar. They estimate the total cost (in 2006), between active care and lost productivity, to have been approximately $100 billion—a number likely to be considerably higher today.
In looking at pharmacologic approaches to low-back pain treatment, acetaminophen was found to be on a par with placebo, offering little benefit but presenting known risks of liver damage. Other drugs, ranging from cox-2 inhibitors to NSAIDs to opioids, offered slightly greater benefits but with concomitantly pronounced risk.
On the other hand, when looking at nonpharmacologic approaches, including exercise, acupuncture, massage, chiropractic, heat therapy, low level laser therapy, and others (tai chi, yoga, ultrasound, etc.), measurable positive outcomes were found with virtually zero risks. The researchers concluded that, given the evidence at hand in the new study and in the older one, that treatment should always begin with nonpharmacologic approaches first, and only those patients who are nonresponsive to them should be considered for drug therapy or invasive medicine.
Specifically, the three recommendations of the study authors are:
- Given that most patients with low-back pain of any type tend to improve over time regardless of treatment type, they should first turn to the most conservative forms of care (massage, spinal manipulation, etc.), and NSAIDs and muscle relaxants can be considered if necessary.
- For patients with chronic low-back pain, the first option should be nonpharmacologic conservative care. Patients in this group respond more strongly to CAM approaches than those in the acute and subacute groups.
- Patients with chronic low-back pain who fail to respond to nonpharmacologic approaches could consider pharmacologic treatment, starting with those products known to present the least risk, and after being educated by their provider about the known risks posed by such products.
These recommendations are in keeping with the Hippocratic Oath: First, do no harm. It is noteworthy to see an MD association admit that CAM approaches to medical care—and here specifically chiropractic is included—offer superior outcomes to standard allopathic medicine. These results were striking enough that they were summarized in the February 14, 2017, edition of the Wall Street Journal
NOTE: this is basically a rehash of a large government study done several years ago. The number one effective treatment for back pain is what chiropractic physicians do every day in their office, spinal adjustments.
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111

IN THE NEWS: DRONE PACKAGE DELIVERY Recently Amazon announced the first drone delivery. They have a select 30 customers that they're using to do test marketing for drone deliveries. The customer in question lived out in the country and the product that he ordered was not touched by human hands. The Internet order was sent to a robot in the warehouse that found the product and delivered it and attached it to the drone. The drone in turn successfully delivered the product to the customer within 13 minutes from click to arrival. Now they just need to mount lasers to deal with the porch pirates that steal newly delivered packages. Welcome to the 21st century.

WELLNESS: GROWING DANGER OF SUPERBUG INFECTIONS For years I've been warning patients against the overuse of antibiotics. Even though the problem in the past was rare, statistics show it's not rare anymore. The 2014 review on antimicrobial resistance made a low estimate that around 700,000 deaths are caused each year because of resistant organisms. As a patient I realize that it is difficult not to follow a doctor's recommendations when they prescribe antibiotics. And if the average doctor was careful in their prescription of antibiotics then we would not be having the problem that we have today. The facts are, most of the time, antibiotics are prescribed unnecessarily. By that I mean there are natural means to effectively resolve the bacterial overgrowth that has led to the infection. The number of natural “antibiotics” is growing every year. Natural antibiotics do not cause antibiotic resistant strains because natural antibiotics are not the same as pharmaceutical antibiotics and they work on a completely different mechanism. The above death statistics from superbug infections will probably start doubling every 5 to 10 years. It's important you make a choice today to keep you and your family safe. Number 1 keep your nervous system free of pressure nd maintain a healthy diet. Number 2 if you believe you have an infection make an appointment so we can evaluate if a natural product would be effective. Most infections are self-limiting. Chiropractic and natural healthcare 1st, drugs 2nd, surgery last.

CHIROPRACTIC: OFFERING SAFER HEALTHCARE The CDC estimates over 2000 people a week die from prescription drugs. Another thousand people die as a result of surgery. A good percent of those surgeries and most of the prescriptions could have been prevented through natural healthcare. The advancement and natural healthcare in the past 40 years has been amazing. If there weren't powerful forces trying to limit patients access to natural healthcare, based on statistics of research done in the late 90s chiropractic and natural healthcare would be the dominant healthcare in the United States. In a American Medical Association's report released in the late 90s showed that more people are seeking doctors who practice natural healthcare than doctors who prescribed drugs and surgery. That initiated major changes in insurance coverage to direct people away from natural healthcare. The American Medical Association does not want its members to have to compete with doctors in the natural healthcare field because studies/statistics show they would lose hands down. Drugs and surgery shine in the emergency room under crisis care conditions. Most health problems are not crisis care conditions and are best served by diet, targeted nutritional therapy, spinal adjustments, exercise and detoxification. Tell your friends about chiropractic.

FUNNY BONE: Late one night a mugger wearing a mask stopped a well-dressed man and stuck a gun in his ribs. "Give me your money," he demanded. Scandalized, the man replied, "You can’t do this – I’m a US Congressman!" "Oh! In that case," smiled the robber, "Give me MY money!"@@ Police officer talks to a driver: Your tail light is broken, your tires must be exchanged and your bumper hangs halfway down. That will be 300 dollars. Driver: Alright, go ahead. They want twice as much as that at the garage.@@ "According to a new estimate, Congress has had a full work week just 14 percent of the time since 1978. Congress said they planned to address the report next week because it's already Tuesday." –Jimmy Kimmel

Visit our web sites: keefeclinic.com-faceebook/keefeclinic.com
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111

IN THE NEWS: Time to Age Gracefully: 6 Tips to Take to Heart Why not try these natural, noninvasive methods instead to make the aging process as smooth and well, natural as possible? It's about adopting lifestyle habits that make you feel good to be alive, no matter what age you are: 1. You are what you eat: And if you eat too much of the wrong stuff, your body will pay for it. 2. Active is awesome: Research links an active life with healthy aging and longevity, for two primary reasons: First, the more activities you involve yourself in (and enjoy), the better you feel. Second, activity in the form of exercise is vital to healthy aging; stay sedentary and your body will break down, create disease and put you exactly where you've spent too much time: lying down. 3. Count some sheep (and get some sleep):Adequate sleep, both quantity and quality, reduces disease risk. 4. Make a few friends (or a whole bunch):Evidence suggests people who maintain healthy relationships and are socially active longer than people who remain isolated with few or no friends. 5. Give your skin a break: From the sun, that is. While a little sun exposure helps produce vitamin D, too much can do tremendous damage, both in the form of skin cancer and general aging of the skin (wrinkling, spotting, dryness, etc.). 6. Stress can be a real killer: We mean it! Chronic stress has been implicated in a wide range of health conditions, and it dramatically impacts your life experience. Who wants to live a long, stressful life?

WELLNESS: Five Things You Can Do To Boost Your Mood Your mood is something that affects many aspects of your health from your heart to your thyroid to your sleep cycle to your menstrual cycle. So, as the daylight hours start to wane this winter season, how can you keep your mood elevated? There are five easy ways to keep your mood elevated this winter season: 1-Stay in touch with your loved ones, When we are surrounded by friends and loved ones, we manage our stressors and mood triggers better. 2-Keep touching your furry friends, Studies suggest that pets bring joy and those with pets feel happier. 3-Light therapy isn't a thing of the past, light therapy during the winter season for seasonal affective disorder HELPS. 4-Keep your kitchen stocked full of vegetables and avoid sugars, if you eat a diet high in antioxidants, minerals and vitamins in the form of vegetables and avoid sugars, your mood will likely be more stable. 5-Keep your body moving throughout the winter season, exercise is always helpful for mood because when you exercise, you release more endorphins and helps to trigger better mood.
CONDITION OF THE WEEK: Shoulder problems can be minor or serious. Symptoms may include pain, swelling, numbness, tingling, weakness, changes in temperature or color, or changes in your range of motion. Shoulder injuries most commonly occur during sports activities, work-related tasks, projects around the home, or falls. Be it a strain or sprain, bursitis, tendinitis, arthritis or subluxation there are many causes for shoulder pain/dysfunction. Chiropractic adjustments of the neck and shoulder, nutritional therapy for the connective tissue and bursa of the shoulder , electrotherapy , pulsed magnetic therapy can all be effective in correcting shoulder problems. Tell someone about chiropractic.

FUNNY BONE: Some people just have a way with words, and other people … oh … not have way.-Steve Martin@@ If people say they just love the smell of books, I always want to pull them aside and ask, To be clear, do you know how reading works?
Visit our web sites: keefeclinic.com&facebook.com/keefeclinic
| Effects of Prone Pelvic Adjustments on Posture |
| The Study: Effects of pelvic adjustment on pelvic posture and angles of the lower limb joints during walking in female university students
The Facts:
a. The authors indicate that the pelvis is important to posture.
b. The subjects were 30 female students from a university.
c. They were divided between a control group which did stretching only and an adjustment group.
d. The adjustments used were performed by physical therapists "in keeping with Gonstead's theory" and consisted of prone adjustments to the PI ilium and also to the AS illium. (emphasis ours)
e. The authors used a BackMapper device which analyses postures in 3D.
f. They found that the adjustment group showed a significant improvements in trunk imbalance, pelvic position, pelvic torsion and also the position of the scapulae while the stretching group showed no significant differences in these same areas..
Take Home:
Prone adjustments of the SI joints changed posture significantly as compared to stretching only.
Reviewer's Comments:
I think that most of us feel that adjustments can change posture and this study reinforces that thought. However there are not a great number of studies other than those done on upper cervical type adjustments that show alignment changes on radiographs due solely to adjustments. I would like you to consider the following: If posture changes then the alignment between boney structures must change. The overall alignment changes must mimic the amount of postural change but how much change occurs at individual segments cannot be determined without imaging. As we say in my world, more research is needed. I love to end things on a self serving note.
Reviewer: Roger Coleman DC
Editor : Mark R. Payne DC
Reference: Cho M, Effects of pelvic adjustment on pelvic posture and angles of the lower limb joints during walking in female university students. See comment in PubMed Commons belowJ Phys Ther Sci. 2016;28:1284-8. doi: 10.1589/jpts.28.1284. Epub 2016 Apr 28
|
Chiropractic as the Solution for Mechanical Spine Failure and Failed Back Surgery.
By: William J. Owens DC, DAAMLP
Mark Studin DC, FASBE(C), DAAPM, DAAMLP
A report on the scientific literature.
The latest CDC statistics show that in 2012, 54 out of 100 people had self-reported musculoskeletal conditions. By way of comparison, that is six times more than self-reported cases of cancer, double that of respiratory disease and one-third more than circulatory disorders. If we extrapolate that to a more current population in the United States of 321 million, that equates to 173 million people reporting musculoskeletal problems in 2012. Many of these are spine patients who suffer long-term without any type of biomechanical assessment or functional case management.
In 2013, Itz, Geurts, van Kleef, and Nelemans reported, “Non-specific low back pain [LBP] is a relatively common and recurrent condition with major medical and economic implications for which today there is no effective cure” (p. 5). The idea that spinal pain has a “natural history” resulting in a true resolution of symptoms is a myth and the concept that spine pain should only be treated in the acute phase for a few visits has no support in the literature. We don’t address cardiovascular disease in this manner, i.e. wait until you have a heart attack to treat, we don’t follow this procedure with dentistry, i.e. wait until you need a root canal to treat, and we certainly don’t handle metabolic disorders such as diabetes in this way, i.e. wait until you have diabetic ulcers or advanced vascular disease to treat. Why does healthcare fall short with spinal conditions in spite of the compelling literature that states the opposite in treatment outcomes?
The front lines of medical care for spine-related pain is typically the prescription of pain medication, particularly at the emergency care level, and then if that doesn’t work, a referral is made to physical therapy. If physical therapy is unsuccessful, the final referral is to a surgeon. If the surgeon does not intervene with surgery, then the diagnosis becomes “non-specific back pain” and the patient is given stronger medication since there is nothing the surgeon can do. In those surgical interventions that result in persistent pain, a commonly reported problem, there is an ICD-10 diagnosis for failed spine surgery, M96.1
A recent article Ordia and Vaisman (2011) described this syndrome a bit further stating the following, “We propose that these terms [post laminectomy syndrome or failed back syndrome] should be replaced with Post-surgical Spine Syndrome (PSSS)” (p. 132). They continued by reporting, “The incidence of PSSS may be reduced by a meticulous neurological examination and careful patient selection. The facet and sacroiliac joints should always be examined, particularly when the pain is predominantly in the lower back, or when it radiates only to the thigh or groin and not below the knee” (Orida & Vaisman, 2011, p. 132). The authors finally stated, “Adherence to these simple guidelines can result in a significant reduction in the pain and suffering, as also the enormous financial cost of PSSS” (Orida & Vaisman, 2011, p. 132). What they are referring to is a careful distinction between an “anatomical” versus a “biomechanical” cause of the spine pain.
According to Mulholland (2008), “[Surgery] Spinal fusion became what has been termed the “gold standard” for the treatment of mechanical low back pain, yet there was no scientific basis for this” (p. 619). He continued, “However whilst that fusion [surgery] may be very effective in stopping movement, it was deficient in relation to load transfer” (Mulholland, 2008, p. 623). He concluded, “The concept of instability as a cause of back pain is a myth. The clinical results of any procedure that allows abnormal disc loading to continue are unpredictable” (Mulholland, 2008, p. 624). Simply put, surgery does not correct the underlying biomechanical failure or the cause of the pain.
When a biomechanical assessment is lacking, the patient’s pain persists and allopathic medicine is focused on “managing the pain” vs. correcting the underlying biomechanical lesion/pathology/imbalance, the medication of choice at this point in care has been opioid analgesics. Back in 2011, the CDC reported, “Sales of OPR quadrupled between 1999 and 2010. Enough OPR were prescribed last year [2010] to medicate every American adult with a standard pain treatment dose of 5 mg of hydrocodone (Vicodin and others) taken every 4 hours for a month” (p. 1489). That was 6 years ago, which was when people began to feel that treating musculoskeletal pain with narcotics was trending in the wrong direction. Now, in 2016, we can see there is a problem of epidemic proportions to the point that MDs are changing how they refer spine patients for diagnosis and treatment.
Dowell, Haegerich, and Chou (2016), along with the CDC, published updated guidelines relating to the prescription of opioid medication:
Opioid pain medication use presents serious risks, including overdose and opioid use disorder. From 1999 to 2014, more than 165,000 persons died from overdose related to opioid pain medication in the United States. In the past decade, while the death rates for the top leading causes of death such as heart disease and cancer have decreased substantially, the death rate associated with opioid pain medication has increased markedly.
…a recent study of patients aged 15–64 years receiving opioids for chronic noncancer pain and followed for up to 13 years revealed that one in 550 patients died from opioid-related overdose at a median of 2.6 years from their first opioid prescription, and one in 32 patients who escalated to opioid dosages >200 morphine milligram equivalents (MME) died from opioid-related overdose. (p. 2)
Clearly, there needs to be a nationwide standard for the process by which patients with spine pain are handled, including academic and clinical leadership on spinal biomechanics. The only profession that is poised to accomplish such a task is chiropractic.
In a recent study by Houweling et al. (2015), the authors reported, “The purpose of this study was to identify differences in outcomes, patient satisfaction, and related health care costs in spinal, hip, and shoulder pain patients who initiated care with medical doctors (MDs) vs those who initiated care with doctors of chiropractic (DCs) in Switzerland” (p. 477). This is an important study which continually demonstrates maintaining access to chiropractic care, for both acute and chronic pain is critical. We can also see from current utilization statistics that chiropractic care is underutilized on a major scale. The authors also state, “Although patients may be comanaged with other medical colleagues or paramedical providers (eg, physiotherapists), treatment for the same complaint may vary according to the type of first-contact provider. For instance, MDs tend to use medication, including analgesics, muscle relaxants, and anti-inflammatory agents, for the treatment of acute nonspecific spinal pain, whereas DCs favor spinal manipulative therapy as the primary treatment for this condition” (Houweling et al., 2015, p. 478). The continue by stating “This study showed that spinal, hip, and shoulder pain patients had modestly higher pain relief and satisfaction with care at lower overall cost if they initiated care with DCs, when compared with those who initiated care with MDs” (Houweling et al., 2015, p. 480). Overall, when taking cost into consideration, “Mean total spinal, hip, and shoulder pain-related health care costs per patient during the 4-month study period were approximately 40% lower in patients initially consulting DCs compared with those initially consulting MDs” (Houweling et al., 2015, p. 481). The authors concluded, “The findings of this study support first-contact care provided by DCs as an alternative to first-contact care provided by MDs for a select number of musculoskeletal conditions” (Houweling et al., 2015, p. 481).
Bases on the literature and outcome studies, backed up with 121 years of doctors of chiropractic and their patients’ testimonies, the time has never been better for the chiropractic profession to move into treating the 93% of the population that is not under care. Chiropractic must be moved from the accepted standard of biomechanical processes in the laboratory to the standard of care for spine beyond fracture, tumor or infection across all professions, inclusive of physical therapy. The outcomes overwhelmingly support that anything less perpetuates the epidemic of failed back treatments.
References
1. Centers for Disease Control and Prevention. (2015). National hospital discharge survey. Retrieved from: http://www.cdc.gov/nchs/nhds.htm
2. United States Census Bureau. (n.d.). Quick facts, United States. Retrieved from https://www.census.gov/quickfacts/
3. Itz, C. J., Geurts, J. W., van Kleef, M., & Nelemans, P. (2013). Clinical course of non‐specific low back pain: A systematic review of prospective cohort studies set in primary care. European Journal of Pain, 17(1), 5-15.
4. Ordia, J., & Julien Vaisman. (2011). Post-surgical spine syndrome. Surgical Neurology International, 2, 132.
5. Mulholland, R. C. (2008). The myth of lumbar instability: The importance of abnormal loading as a cause of low back pain. European Spine Journal, 17(5), 619-625.
6. Centers for Disease Control and Prevention. (2011). Vital signs: Overdoses of prescription opioid pain relievers - United States, 1999--2008. Morbidity and Mortality Weekly Report, 60(43), 1487-1492.
7. Dowell, D., Haegerich, T. M., & Chou, R. (2016). CDC guideline for prescribing opioids for chronic pain - United States, 2016. JAMA, 315(15), 1624-1645.
8. Houweling, T. A., Braga, A. V., Hausheer, T., Vogelsang, M., Peterson, C., & Humphreys, B. K. (2015). First-contact care with a medical vs chiropractic provider after consultation with a swiss telemedicine provider: Comparison of outcomes, patient satisfaction, and health care costs in spinal, hip, and shoulder pain patients. Journal of Manipulative and Physiological Therapeutics, 38(7), 477-483.
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111

IN THE NEWS: What is alkaline water and can it really help with heartburn? You may have noticed the buzz about alkaline water recently: It’s a staple of the alkaline diet, and promoted by celebs like Miranda Kerr for its supposed health perks. Among those perks is the belief that alkaline H2O—which, by definition, has a higher pH (and lower acidity) than what comes out of the tap—can help neutralize stomach acid and relieve symptoms of gastroesophageal reflux, aka heartburn. NOTE: though this article was interesting and it does show benefits for heartburn that’s not the primary purpose of alkaline water. Alkaline water is one tool along with other foods and drinks to change your pH to more normal setting. Both urine and saliva should be 6.4. When your urine pH gets down to 5.5 or below this puts your body under stress. One of the things that happens is you start leeching alkaline minerals from your bone and teeth. So alkaline water can be an important tool if you system is hyper acidic which usually means it’s inflamed.

WELLNESS: The secret to surviving a heart attack? Eating plenty of salmon, pecans and vegetable oils 'lowers chances of dying' Oily fish like mackerel, salmon and sardines have high levels of omega-3, Some nuts, seeds and oils contain high levels of plant-based equivalent, Study looked at research based on more than 45,000 patients globally. These foods reduce inflammation in the body which is the latest scientific understanding for heart disease. The cholesterol theory for heart disease has never once been proven through scientific studies in the past 50 years. Unfortunately sometimes politics and fraud produce practices that takes years to expose and change. If you’re taking drugs for cholesterol your shortening your life span. Change your diet and lifestyle and you can substantially reduce your likelihood of having a heart attack. Note: Ask for list of anti-inflammatory foods.
CHIROPRACTIC: The neurological bases for neck and arm symptoms Your neck contains the smallest vertebrae in your spine with the least amount of support. Neck problems can arise from simple headdown posture to whiplash type injuries. When these bones lose their proper position and balance they can stress the delicate nerves that travel into the muscles and tissues of the neck and on down the arm to the tip of the fingers. This can be the source of neck pain, stiffness, limited rotation and problems sleeping. These nerves also innervate the shoulder and can lead to different types of shoulder dysfunction, the elbow leading to tennis elbow type symptoms, the wrist leading to carpal tunnel syndrome and into the fingers leading to grip strength issues, numbness and tingling within the hand. Medications, of course, do not realign the spine. And suppressing symptoms thus allowing misalignments to remain are the source of long-term degenerating processes like arthritis and disc disease. Chiropractic offers the safest most direct method of restoring a strong healthy neck. If you or someone you know suffers from neck or arm symptoms tell them about chiropractic.

FUNNY BONE: Ambition is a poor excuse for not having enough sense to be lazy.@@ We are all here on earth to help others; what on earth the others are here for I don't know.
Visit our web site: keefeclinic.com-ebook/keefeclinic.com
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111
American Chiropractic Association (ACA) has announced a national health care observance
October is
National Chiropractic Month

DO YOU KNOW SOMEONE WITH A HEALTH PROBLEM OR IN PAIN?
INVITE YOUR FAMILY OR FRIENDS TO THE PARTY
Who do you know who is hurting? Who do you know that you have been trying to get started at Keefe Clinic?
Now is the time to get your spouse, or child started on the road to good health.
Complimentary
DIAGNOSTIC WORK UP DURING OCTOBER
Complimentary initial exam and one X-ray.
Tell someone today
IN THE NEWS: Environmental Exposures, Autism and Developmental Delays — An Approach From an Integrative Psychiatrist estimated 1 in 50 American children. The number of children with autism has increased by an alarming rate over the last 20 years and will likely continue. A growing number of children also struggle with developmental and speech delays, as well as motor disorders. According to the latest statistics, developmental delays affect 1 out of 6 or 7 children. Environmental exposure are a significant factor that can contribute to the development of ASD and other developmental delays. There are many safe, gentle treatment options, including dietary changes and eliminating toxic exposures. ASK ABOUT DETOX!
LINK: peeling-the-onion/
Courtesy of:
John H. Keefe III, D.C.
(918) 663-1111

IN THE NEWS: UTIs Are Horrible and Soon There Will Be No Drugs That Can Help You A superbug that can shake off a last-ditch antibiotic called colistin has been alarming the global health community since 2015. It first turned up in hogs on a Chinese farm and has since been found in 30 other countries, including the United States. According to a new paper by Rutgers and Columbia University researchers, colistin-resistant E. coli has been here since August 2014 at the latest—and the particular strain they found is also resistant to another family of last-resort antibiotics, carbapenems. It's also chilling that this superstrain of E. coli turned up in a UTI case. E. coli is the most common trigger of UTIs, which in turn are "among the most common infections in people," according to the Centers for Disease Control and Prevention. Note: I have been warning patients about this problem for the past 30 years. About 23 years ago the “Journal of the American Medical Association” gave one whole publication to this issue discussing what can be done. One of the solutions which would’ve probably stopped this problem was to make it illegal for the average medical doctor to prescribe antibiotics. Even after multiple warnings sting operations have found a number of medical doctors giving antibiotics to a whole host of conditions that have been shown not to be helped by antibiotics. They just wanted to feel like a doctor who had a solution. So it’s up to the individual patient to protect themselves and their families. Recently the FDA has talked about removing antibacterial soaps from the market because they contribute to superbug development. The good news is natural approaches are still quite effective in most of these cases. Always try a natural approach first when you have an infection you can always go to more aggressive approaches if necessary.
CHIROPRACTIC/WELLNESS: Cloudy with a chance of pain? Wet weather and a lack of sunshine DOES make chronic pain worse It's long been said that cold, damp, weather can make aches and pains worse. Now doctors investigating whether there really is a link between the weather and pain believe it's more than just an old wives' tale. Bad weather - particularly rain and a lack of sunshine - can make chronic pain worse, initial findings of a large study suggests. Medics have asked thousands of sufferers across the country to take part in their research by providing data using their mobile phones. As the number of sunny days increased from February to April, the amount of time spent in severe pain decreased. But pain levels increased again in June when the weather was wetter and there were fewer hours of sunshine, the University of Manchester-led project found. Good news: these issues can be resolved through nutritional therapy and light therapy. You can get full-spectrum light bulbs at the health food store that can supply you with the type of light the sun gives off. Just like with nutritional deficiencies you can have light deficiencies. With Vega testing we can help find the nutrients that can eliminate these weather-related symptoms.

FUNNY BONE: We’ve begun to long for the pitter-patter of little feet, so we bought a dog. It’s cheaper, and you get more feet.@@ People in sleeping bags are the soft tacos of the bear world.@@ I was editing classified ads for a small-town newspaper when a man called to place an ad. "It should read," he said, "‘Free to good home. Golden retriever. Will eat anything, loves children.’"
Visit our web site: keefeclinic.com-faceebook/keefeclinic.com











































































